
How Is A Medical Claims Virtual Assistant Useful In 2026
In the high-pressure world of U.S. healthcare, administrative burdens continue to challenge providers in 2026. Physicians and staff spend countless hours on paperwork instead of patient care—research shows that physicians spend about 33.4% of their work time on administrative and non-patient-facing tasks, while claim denials erode revenue and delay cash flow. A medical claims virtual assistant offers a practical, scalable solution by handling insurance verification, claims submission, follow-up, and denial management remotely or through AI-enhanced tools.
These specialized assistants—whether human virtual professionals or AI-powered systems—integrate with electronic health records (EHRs) and practice management software to automate repetitive tasks. As healthcare faces rising costs and complex payer rules, the best medical claims virtual assistant combines accuracy, compliance, and speed to help practices thrive.
The Growing Challenge of Medical Claims Processing in 2026
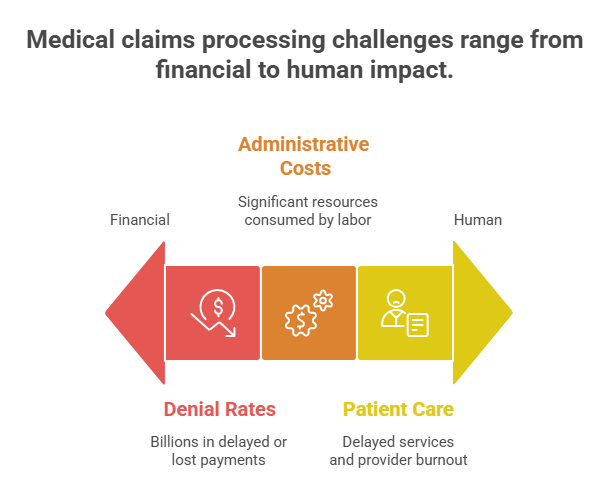
U.S. healthcare providers face persistent administrative hurdles in claims processing amid evolving regulations and payer scrutiny. High denial rates and mounting overhead costs strain operations and impact financial stability. A medical claims virtual assistant helps address these issues by improving efficiency and accuracy in the revenue cycle.
1. Rising Claim Denial Rates and Revenue Impact
U.S. healthcare providers face persistent claim denial issues. In recent 2025-2026 data, initial denial rates average around 11-12% industry-wide, with some segments like commercial inpatient claims reaching 21%. These denials result in billions in delayed or lost payments, with final denial rates rising to about 2.7% and contributing to over $48 billion in net revenue losses across providers. A medical claims virtual assistant tackles these by ensuring clean claims through pre-submission scrubbing, accurate coding, and timely follow-up, directly improving first-pass acceptance rates.
2. Administrative Costs Burdening Practices
Healthcare administrative expenses remain substantial. Labor and billing processes consume significant resources while practices lose productivity as staff handle eligibility checks, appeals, and payment posting. Virtual assistants reduce overhead by operating remotely without the costs of full-time onsite employees, including benefits and office space. This cost-efficiency proves especially valuable amid staffing shortages and rising employer compensation costs.
3. Impact on Patient Care and Provider Burnout
Delayed claims strain practice finances and can lead to higher patient bills or postponed services. Providers experience frustration with prior authorizations and appeals, contributing to burnout. A medical claims virtual assistant shifts this administrative load, allowing clinicians to focus on medicine while improving patient satisfaction through faster resolutions and better cash flow.
Key Ways a Medical Claims Virtual Assistant Delivers Value
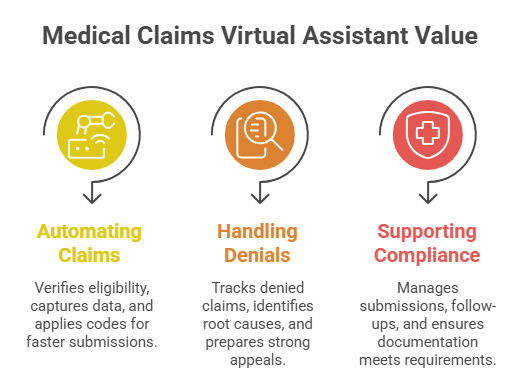
A medical claims virtual assistant provides targeted support across the revenue cycle, helping U.S. practices overcome billing complexities in 2026. By combining automation with specialized expertise, these assistants reduce errors and accelerate reimbursements. Practices benefit from improved efficiency and more time dedicated to patient care.
1. Automating Claims Submission and Reducing Errors
One core strength is end-to-end claims automation. A medical claims virtual assistant verifies patient insurance eligibility in real time, captures accurate data, and applies correct codes. This leads to faster submissions and higher clean claim rates, with practices often seeing notable reductions in accounts receivable days.
2. Handling Denial Management and Appeals Efficiently
Denials require prompt and accurate appeals with payer-specific documentation. Virtual assistants track denied claims, identify root causes, and prepare strong appeals. AI-enhanced versions predict denial risks, allowing proactive corrections that minimize revenue leakage and shorten the reimbursement cycle.
3. Supporting Prior Authorization and Compliance
Prior authorizations remain a major bottleneck in healthcare. Virtual medical assistants manage submissions and follow-ups while ensuring documentation through the assistant meets all the requirements. They help maintain compliance with HIPAA, CMS rules, and payer policies, reducing delays in patient care and risks of audits.
AI-Powered Medical Claims Virtual Assistants: The 2026 Game-Changer
AI integration is transforming medical claims virtual assistants in 2026, enabling predictive analytics and automation. Over 70% of healthcare organizations are expected to adopt AI in revenue cycle management by 2026, reflecting rapid growth. Hybrid models that combine AI speed with human oversight deliver the best results for complex U.S. healthcare billing.
- AI analyzes vast datasets to flag potential issues like eligibility gaps or coding mismatches before submission.
- Predictive models forecast denial risks using historical data for proactive corrections.
- Natural language processing extracts information from clinical notes to support accurate coding.
- AI processes routine claims faster than manual methods, often reducing processing time significantly.
- Hybrid AI-human systems balance high-volume efficiency with nuanced handling of exceptions and appeals.
Choosing the Best Medical Claims Virtual Assistant in 2026
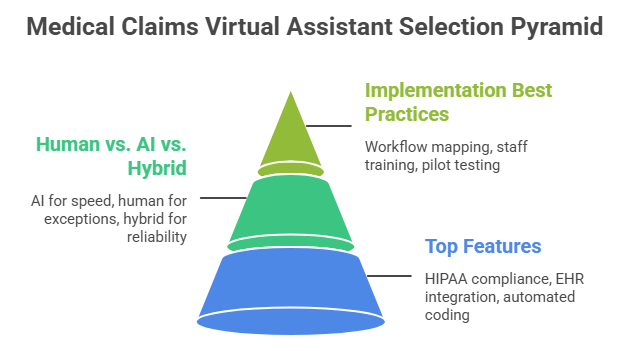
Selecting the right medical claims virtual assistant requires evaluating features, integration capabilities, and alignment with practice needs in 2026. The best options offer scalability and strong support for American healthcare providers. Careful implementation ensures maximum return on investment through improved revenue cycle performance.
1. Top Features
When selecting the best medical claims virtual assistant, prioritize HIPAA-compliant platforms with seamless EHR integration, real-time eligibility verification, and automated coding support. Additional must-haves include denial analytics, robust reporting, and multi-payer rule engines for scalability across practice sizes.
2. Comparing Human vs. AI vs. Hybrid Options
Human virtual assistants excel in handling exceptions and building payer relationships. AI solutions provide superior speed and volume handling for routine tasks. Hybrid approaches deliver the most reliable outcomes by combining AI efficiency with human expertise for complex medical claims.
3. Implementation Best Practices
Successful adoption starts with clear workflow mapping and staff training. Pilot testing on high-volume tasks like eligibility checks helps minimize disruption. Regular performance reviews based on key metrics ensure ongoing optimization and strong ROI.
Cost Considerations and Medical Claims Virtual Assistant Pay
Understanding pricing and potential savings is essential when evaluating a medical claims virtual assistant for your practice in 2026. Costs vary by model, but the investment often delivers quick returns through reduced denials and lower overhead. Many providers find significant net savings compared to traditional in-house staffing.
- Human virtual assistant services typically range from $8-25+ per hour or use monthly retainers based on scope and expertise.
- AI-powered tools operate on subscription models scaled to claim volume, proving cost-effective for higher volumes.
- Hybrid solutions combine automation with human oversight for optimized expenses and performance.
- Practices can achieve notable ROI through 20-30% improvements in collections and reduced administrative staffing needs.
- Medical claims virtual assistant pay for professionals often aligns with specialized billing roles, offering flexibility without onsite overhead costs.
Addressing Common Concerns and Risks
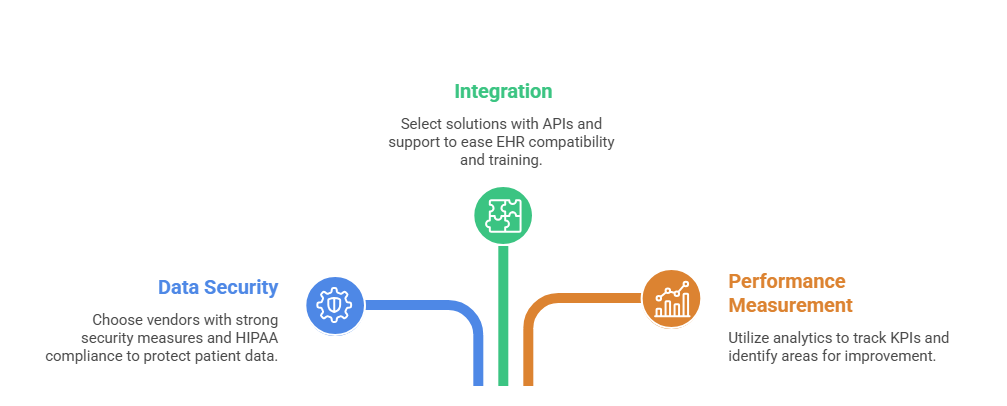
Healthcare providers often have valid concerns when adopting a medical claims virtual assistant. Addressing data security, integration, and performance measurement upfront builds confidence in the solution. Reputable services prioritize compliance and support to ensure smooth operations in 2026.
1. Data Security and HIPAA Compliance
Reputable virtual assistant services use encrypted platforms and adhere strictly to HIPAA regulations. They maintain business associate agreements and undergo regular audits to protect sensitive patient data. Choosing established vendors with strong security track records helps maintain compliance and patient trust.
2. Integration Challenges and Training Needs
EHR compatibility can present initial hurdles during setup. Modern solutions provide APIs and dedicated implementation support to ease transitions. Comprehensive training for in-house teams ensures smooth handoffs and maximizes the benefits of the virtual assistant.
3. Measuring Success and Continuous Improvement
Track key performance indicators such as denial rate reduction and average reimbursement time. Built-in analytics help monitor progress and identify areas for refinement. Regular reviews and feedback loops allow practices to adapt to changing regulations and sustain long-term gains.
How virtual assistants help in Medical Claim Service
Virtual assistants play a crucial role in simplifying the complex world of medical claims processing for U.S. healthcare practices in 2026. By handling repetitive and detail-oriented tasks with accuracy and speed, they significantly reduce administrative burden while improving overall revenue cycle efficiency. From eligibility checks to denial management, these professionals help providers focus more on patient care and less on paperwork.
- They perform real-time insurance eligibility verification to prevent submission of invalid claims and reduce upfront denials.
- Virtual assistants handle accurate CPT, ICD-10 coding, and claims scrubbing for higher first-pass acceptance rates.
- They manage full denial tracking, root cause analysis, and preparation of payer-specific appeals to recover lost revenue faster.
- They streamline prior authorization requests and follow-ups, minimizing delays in patient care and related claim rejections.
- They ensure ongoing compliance with HIPAA, CMS guidelines, and evolving payer rules while maintaining detailed audit-ready documentation.
- They integrate with EHR and practice management systems to automate data entry, payment posting, and reporting for end-to-end efficiency.
TaskVirtual: Your Partner in Medical Claims Virtual Assistant Services
Managing complex medical claims processing, insurance follow-ups, and denial appeals can overwhelm healthcare practices in 2026. From verifying patient eligibility across multiple payers to preparing accurate documentation and handling appeals, these tasks consume significant staff time and impact revenue flow. TaskVirtual provides expert medical claims virtual assistant services that simplify the entire revenue cycle by supporting claims submission, denial management, and compliance requirements with precision and speed.
1. Expert Consultation and Review
TaskVirtual’s skilled virtual assistants assist in insurance verification, accurate coding, claims scrubbing, and timely follow-up while identifying patterns in denials to improve future submissions and maximize reimbursements.
2. Affordable and Flexible Pricing
Hiring a full-time personal assistant can be expensive, but TaskVirtual makes it cost-effective. With pricing plans starting from just $3.12/hour to $14.99/hour, their services are budget-friendly and accessible to healthcare practices of all sizes.
3. Comprehensive Medical Claim Support Solutions
From real-time eligibility verification and clean claim submission to denial tracking and payer-specific appeals, TaskVirtual covers the full spectrum of medical billing and consulting tasks. Their scalable services adapt to whether you need occasional support or complete revenue cycle management.
4. Ongoing Support and Quality Assurance
TaskVirtual goes beyond basic processing by offering continuous monitoring, proactive denial prevention, and regular performance updates. Their dedicated support ensures claims are handled efficiently while maintaining full compliance and accuracy.
5. Proven Track Record of Excellence
With 364 positive reviews and a 4.7-star rating on trusted VA platforms, TaskVirtual is recognised as a reliable partner worldwide. Clients count on their expertise to streamline medical claims processing and improve practice revenue.
FAQ Section
1. What is a medical claims virtual assistant?
A medical claims virtual assistant is a remote or AI-powered specialist who manages insurance verification, claims submission, coding, follow-up, and denial appeals for healthcare practices.
2. How much does a medical claims virtual assistant cost?
Pricing varies from $8-25+ per hour for human VAs to subscription models for AI tools, with savings offsetting costs through fewer denials.
3. Can a medical claims virtual assistant reduce claim denials?
Yes, accurate processing and proactive checks can significantly lower denial rates, with AI versions offering up to substantial reductions.
4. What are the benefits of the best medical claims virtual assistant?
It delivers faster reimbursements, lower administrative costs, reduced errors, better compliance, and more time for patient care.
5. Is AI replacing human medical claims virtual assistants in 2026?
AI augments humans in hybrid models, handling routine tasks while people manage complex cases and oversight.
6. How do I find a medical claims virtual assistant phone number or service?
Contact reputable agencies or platforms via their websites for consultations, demos, and support line details.
Conclusion + CTA
In 2026, a medical claims virtual assistant stands out as a powerful ally for U.S. healthcare providers battling administrative overload, high denial rates, and rising costs. By automating routine processes and leveraging AI for smarter decision-making, these solutions enhance revenue cycle performance and reduce burnout.
Practices that embrace the best medical claims virtual assistant—whether AI-driven, human-supported, or hybrid—gain faster payments, fewer errors, and greater operational resilience. This positions them for success in a complex reimbursement landscape while supporting better patient outcomes. Ready to transform your medical billing? Contact a trusted provider today for a free assessment or demo. Explore how a tailored medical claims virtual assistant can fit your practice size and specialty to reclaim time and revenue.
Sources
- Experian Health State of Claims Report (2025)
- Kodiak Solutions Revenue Cycle Reports (2025-2026 data)
- BLS Occupational Outlook Handbook for Medical Assistants
- Industry analyses on AI in the Revenue Cycle Management market growth
- Various authoritative healthcare RCM benchmarks and denial statistics reports
For more such content, follow our website.







